What is Glaucoma?
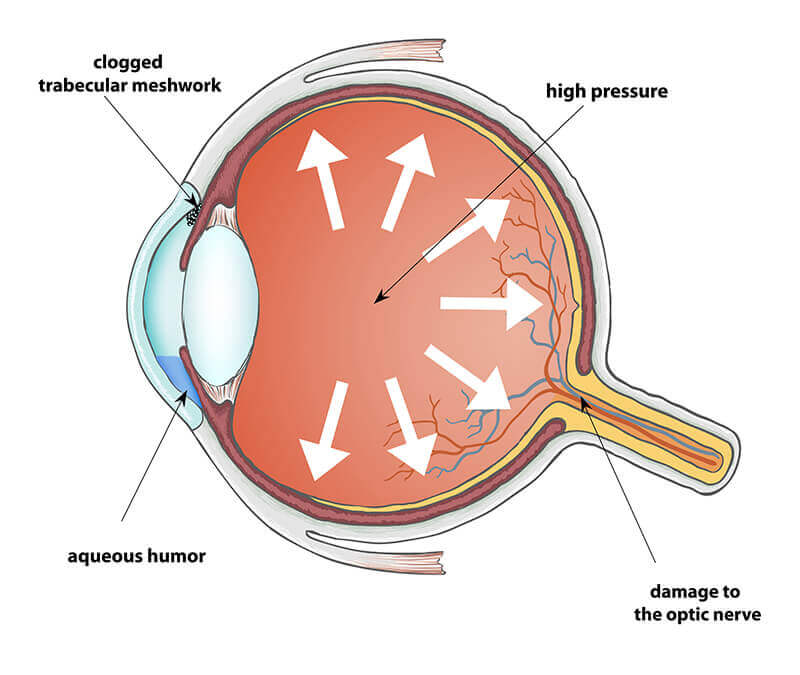
Glaucoma is an eye disease caused by elevated eye pressures that damage the optic nerve. Although the upper limit of “normal eye pressure” is around 21 mmHg, glaucoma can develop at various pressure ranges.
Elevated eye pressure is detrimental to the health of the optic nerve and in time can cause progressive damage. Because the optic nerve does not regenerate or recover, as increasing damage occurs to the optic nerve, the loss of vision quickly accelerates. Typically glaucoma vision loss begins in the peripheral field of vision.
How is glaucoma treated?
The main goal of glaucoma therapy is to lower the eye pressure to halt further damage to the optic nerve.
Traditionally, eye drops have been utilized as a first-line treatment protocol to lower the eye pressure. Different classes of eye drops work in different ways to lower the eye pressure. Some suppress the production of fluid entering the eye; others increasing fluid outflow. Some drops are capable of both mechanisms.
Although eye drops seem simple, in actuality many patients fail to adhere to the regimen consistently. In many cases, poor compliance decreases the efficacy of treatment and damage to the optic nerve and vision progress. Many eye drops carry undesirable side effects or result in allergic responses. Costs of treatment are also an issue as newer eye drops are often not covered by insurance plans.
SLT Laser therapy for Glaucoma
SLT laser therapy is being used earlier in glaucoma therapy as the treatment is well tolerated and repeatable. In some patients with mild glaucoma SLT can be used instead of drop therapy. In more advanced glaucoma, a combination of drops and SLT is needed to keep the eye pressures low. Most SLT treatments will last 3-5 years and this procedure is repeatable. The procedure takes less than five minutes and is virtually painless with topical anesthetics.
Micropulse Transcleral Laser Cyclophotocoagulation for Glaucoma (CPC)
For patients with more advanced glaucoma, a stronger laser can be helpful to lower the eye pressure. CPC lasers suppress the organ that secretes fluid in the eye. The treatment takes less than five minutes and utilizes deeper intravenous anesthetic.
Trabeculectomy
Trabeculectomy is recommended when the ocular pressures cannot be controlled with drop therapy or laser therapy. This surgery involves making a small surgical opening directly into the eye to allow the eye fluid to drain out and be absorbed under the clear tissue those overlays the white of the eye. The tissue overlying the opening will form a blister-like structure. Although this procedure does not involve any implanted hardware scarring can limit its effectiveness. Rarely it may decrease the pressure too much, which can be detrimental to the vision as well. Some patients may feel elevated blister. The surgery lasts 45 minutes and is done under IV sedation and local anesthetic.
Glaucoma Tube Shunts
When a trabeculectomy fails, a tube shunt may be recommended. A shunt is inserted into the eye and attached behind the eye to a small plate covered by the clear tissue that overlays the white of the eye. The pressure lowering is similar to a trabeculectomy. Because of the hardware involved, it is possible to induce side effects such as double vision. This procedure can be vulnerable to infection and exposure of the hardware.
MIGS Glaucoma Surgery (Micro Invasive Glaucoma Surgery)
Because of the potential side effects and complications associated with trabeculectomy and tube shunts, a number of less invasive glaucoma procedures have been developed to prevent the need for more invasive surgeries. These newer procedures are associated with fewer risks and side effects but typically result in less pressure decrease. MIGS procedures aim to be preventative in the need for trabeculectomies and tube shunts further down the line.
iStents MIGS
iStents are tiny stents that can be inserted in the trabecular meshwork of the eye to increase direct drainage of aqueous fluid from the eye and lower the eye pressure. Currently, iStents are only approved for patients with glaucoma who are also having simultaneous cataract surgery. This procedure is quick and virtually pain-free, adding 5-7 minutes to the typical duration of cataract surgery. Both procedures are performed under twilight sedation.
Trabeculotomy MIGS
A trabeculotomy involves opening the eye’s trabecular meshwork so fluid can flow directly into it and lower the eye pressure. The surgery lasts 10 minutes and is done under IV sedation in the operating room. No implanted hardware is involved and this procedure can be performed independently of cataract surgery.
Xen Gel stent MIGS
The Xen Gel stent is a micro tube inserted into the eye and positioned with one end inside the eye and the other end outside the eye, covered by the clear covering over the white of the eye. This tube is microscopic compared to traditional tube shunts and healing is quicker and more stable. This procedure is FDA-approved and is well covered by traditional Medicare plans but considered experimental by Medicare Advantage and traditional commercial insurances.





